Sleep Apnea Treatment Options in 2026: CPAP Therapy vs. Oral Appliance Therapy
If someone has ever joked that your snoring sounds like a freight train, it might not actually be a joke. And if you wake up exhausted after eight hours in bed, that’s another clue. What many people brush off as “poor sleep” is often something more serious: Obstructive Sleep Apnea (OSA).
Sleep doctors see this every day. Untreated OSA quietly chips away at your health. During sleep, the airway collapses, breathing stops, oxygen drops, and the body reacts instantly. Heart rate spikes. Stress hormones surge. Then breathing resumes—until it happens again. And again.
Night after night, sometimes hundreds of times.
That constant cycle puts real strain on the body. Over time it dramatically raises the risk of stroke, Type 2 diabetes, hypertension, and congestive heart failure. Snoring is just the surface symptom. The real problem is what’s happening inside the body while you sleep.
The good news? Sleep medicine has evolved quickly. By 2026, diagnosing and treating sleep apnea looks very different from what patients experienced a decade ago.
No more wires everywhere. No more uncomfortable nights in a sleep lab for most people. Technology has simplified the process—and made treatment far easier to stick with.
Home Sleep Testing: The New First Step
For years, diagnosing sleep apnea meant one thing: an overnight sleep study called polysomnography. You’d show up at a clinic in the evening, get connected to a tangle of sensors, and attempt to sleep while technicians monitored everything from another room.
Not exactly relaxing.
Today, that process has changed. Home Sleep Testing (HST) has become the starting point for most patients.
What an At-Home Sleep Test Looks Like Now
Modern at-home sleep apnea tests are surprisingly simple. Typically, the system includes a small wearable device—often worn on the wrist or finger—and sometimes a lightweight chest sensor.
That’s it.
These devices collect the key metrics doctors need:
- Heart rate patterns
- Blood oxygen levels (SpO₂)
- Breathing effort
- Sleep-related respiratory events
You wear the device for one night in your own bed. The next morning, the data uploads automatically through a secure platform so your physician can review it.
No lab. No cameras. No strange environment interfering with your sleep.
Insurance Coverage Is Driving the Shift
Another reason home sleep testing has exploded in popularity is insurance policy changes. Major insurers such as Aetna, Cigna, and UnitedHealthcare now frequently recommend HST as the first diagnostic step when sleep apnea is suspected.
Coverage under Medicare has also become more straightforward. Patients who meet specific screening criteria can now qualify for reimbursement without jumping through as many administrative hoops.
Cost has dropped as well. A decade ago, an overnight lab study could run well over a thousand dollars. In contrast, many home sleep tests in 2026 fall somewhere between $150 and $250.
For patients, the difference is obvious: faster access, lower cost, and far less inconvenience.
CPAP Therapy in 2026: Smaller, Smarter, and Much Quieter
Once sleep apnea is diagnosed, treatment usually begins with Continuous Positive Airway Pressure, better known as CPAP.
If you’re picturing the loud, bulky machines people used ten or fifteen years ago, forget that image. CPAP technology has improved dramatically.
Today’s CPAP Machines Are Practically Silent
Noise used to be a major complaint. Older CPAP machines hummed loudly through the night, sometimes keeping partners awake.
Modern systems are a different story.
The quietest CPAP machines in 2026 operate below 20 decibels—roughly the volume of a whisper. Manufacturers achieved this through better acoustic insulation and highly efficient brushless motors.
Most patients barely notice the device once it’s running.
Comfort Features That Actually Matter
Comfort determines whether someone sticks with therapy. And manufacturers know it.
Today’s CPAP units usually include:
- Built-in heated humidifiers
- Heated tubing to prevent condensation (“rainout”)
- Automatic pressure adjustments
- Remote monitoring capabilities
The heated humidifier alone solves one of the biggest complaints from early CPAP users—dry mouth and throat irritation.
But the real leap forward is Auto-CPAP technology. These systems use advanced algorithms to adjust air pressure breath-by-breath. If your airway begins to collapse, the machine increases pressure slightly. When breathing stabilizes, pressure drops again.
The result: you receive exactly the support needed, nothing more.
Many machines also transmit usage data through cellular connections. Sleep specialists can review therapy performance and adjust settings remotely, without requiring patients to visit the clinic.
Oral Appliance Therapy: A Simple Alternative
Despite all these improvements, some people simply cannot tolerate a CPAP mask. It happens.
Masks can feel restrictive. Some patients feel claustrophobic. Others remove the device in their sleep without realizing it.
That’s where Oral Appliance Therapy (OAT) comes in.
For patients with mild to moderate sleep apnea, oral appliances often provide a practical alternative.
How Oral Appliances Work
An oral appliance looks similar to a sports mouthguard or orthodontic retainer. But its purpose is very specific.
The device gently shifts the lower jaw (mandible) forward during sleep. This small adjustment keeps the airway open by preventing the soft tissues in the throat from collapsing backward.
It’s a simple mechanical solution—and for many patients, surprisingly effective.
Why Many Patients Stick With It
Here’s the reality: the best sleep apnea treatment is the one you actually use.
CPAP therapy can be extremely effective when worn consistently. But adherence has always been the challenge.
Oral appliances remove many of the barriers that cause people to abandon treatment:
No noise.
There’s no motor, no airflow, no humming sound.
Freedom to move.
You can sleep on your back, side, or stomach without worrying about hoses or masks shifting.
Travel convenience.
The device fits in a small case and doesn’t require electricity. Frequent travelers love this. So do campers and people who spend time off-grid.
For the right patient, that simplicity makes all the difference.

CPAP vs. Oral Appliance: Which One Makes Sense?
There isn’t a universal answer. Choosing between CPAP therapy and an oral appliance depends on a few key factors.
| Feature | CPAP Therapy | Oral Appliance Therapy |
| Best for | Moderate to severe OSA | Mild to moderate OSA |
| Effectiveness | 95–100% when used properly | 75–85% depending on anatomy |
| Portability | Requires machine and power source | Small, travel-friendly device |
| Maintenance | Regular cleaning of mask and parts | Simple brushing or soaking |
| Initial cost | $800 – $1,800 | $1,500 – $3,000 (custom-made) |
| Long-term adherence | Moderate | Often higher |
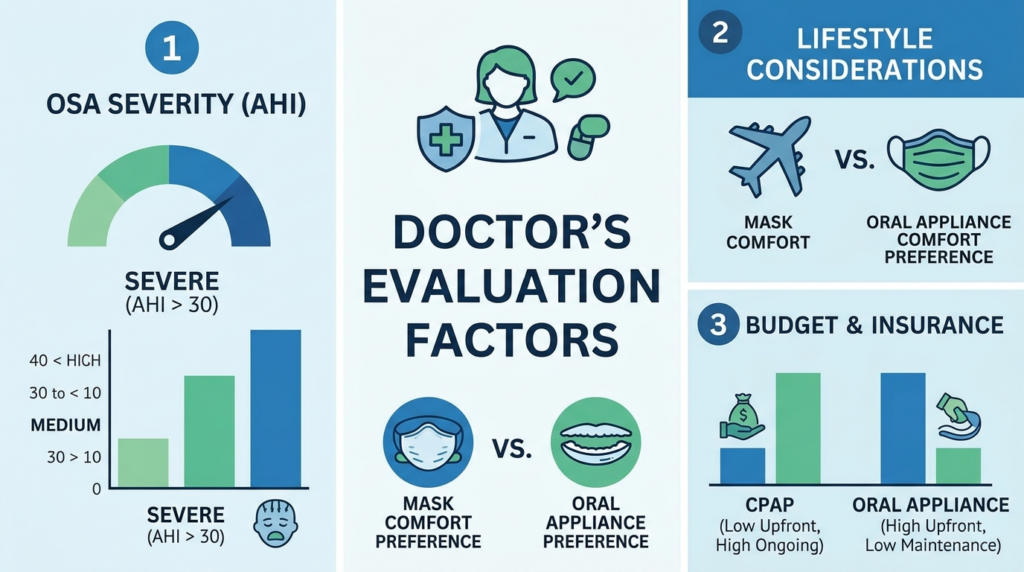
What Doctors Look At
Severity of sleep apnea
The Apnea-Hypopnea Index (AHI) matters. When AHI exceeds 30—classified as severe OSA—CPAP therapy remains the most reliable starting point. The positive airway pressure physically prevents airway collapse.
Lifestyle considerations
Patients who travel frequently or struggle with mask discomfort often prefer oral appliances. Convenience matters more than people expect.
Budget and insurance coverage
CPAP systems generally cost less upfront but require ongoing supplies such as masks, filters, and cushions. Oral appliances cost more initially because they must be custom-fit by dental specialists, but long-term maintenance costs are usually lower.
The Real Goal: Protecting Your Health
Treating sleep apnea isn’t just about stopping snoring. The real objective is protecting the body—especially the brain and heart—from years of repeated oxygen deprivation.

The difference after treatment can be dramatic.
Patients often report clearer thinking, steadier moods, and energy levels they haven’t felt in years. Morning headaches disappear. Brain fog lifts. Even blood pressure can improve once sleep becomes stable again.
None of that happens, though, until the condition is properly diagnosed.
If sleep apnea is even a possibility, the smartest move is simple: get tested. A quick risk assessment or a home sleep test can provide the answers.
From there, a sleep specialist can help determine whether CPAP therapy or an oral appliance makes the most sense for your situation.
Better sleep isn’t a luxury. It’s a medical necessity. And in 2026, getting the right treatment is easier than it’s ever been.
